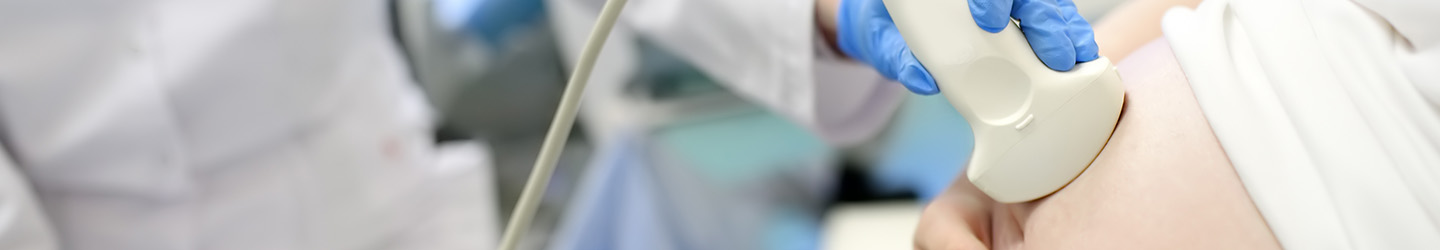
Robotic Surgery
Robotic Surgery
Incredibly precise for complex operations, robot-assisted surgeries completed by Dr. Jacob get patients quickly on the mend and can help solve couples’ infertility issues.
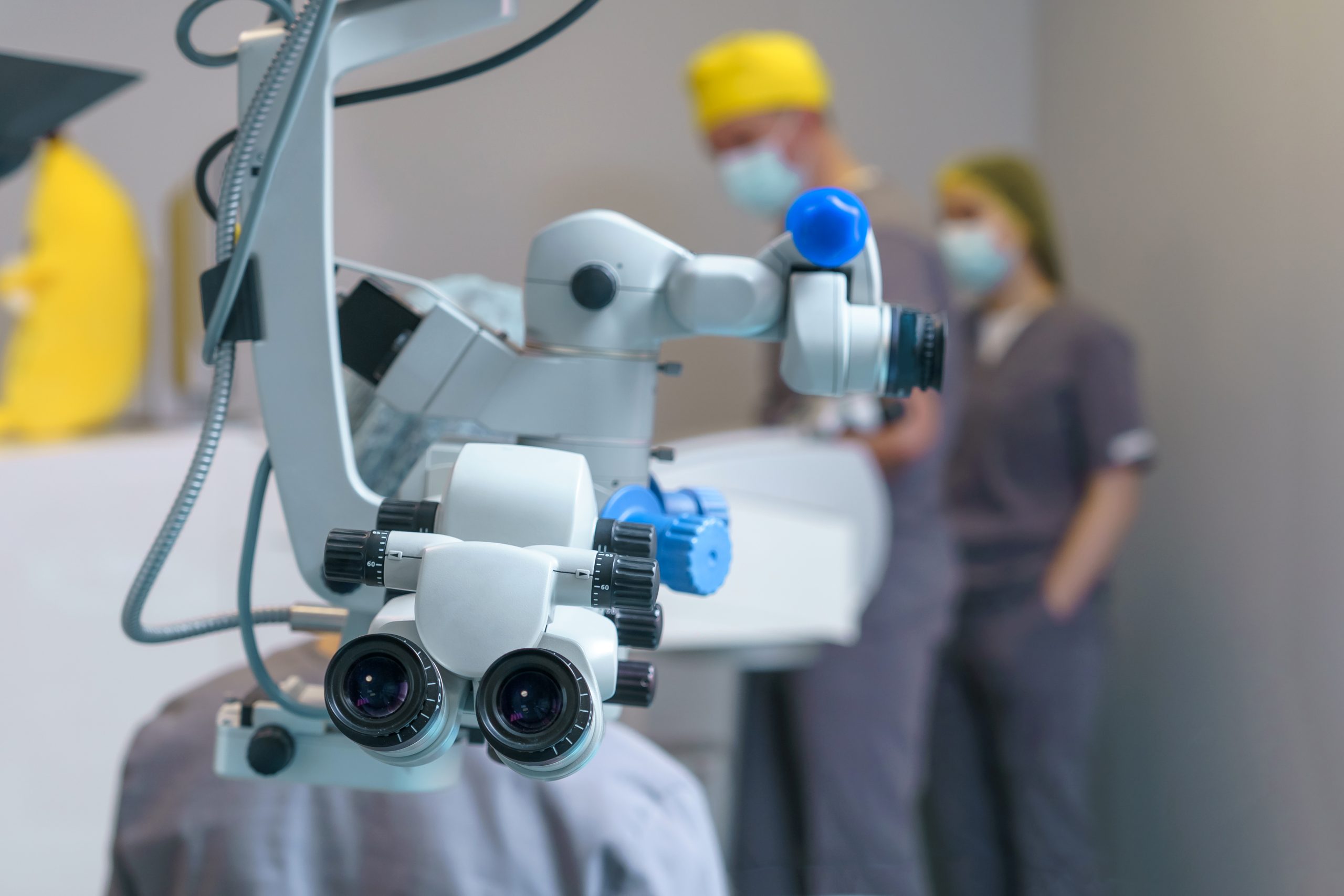
Also known as robot-assisted surgery, robotic surgery is a high-tech system enabling surgeons around the globe to delicately perform minimal access procedures with excellent precision.
At GoFertility (CRMRS) in Creve Coeur, Dr. Saji Jacob — a certified robotic surgeon who doubles as a national proctor to train doctors around the country in robotic OB/GYN procedures — routinely performs numerous robot-assisted surgeries to quickly get our patients on the mend. Since CRMRS’s opening in 2011, Dr. Jacob has completed more than 1,000 robotic surgeries. He specializes in complex gynecological procedures including:
- Myomectomies or fibroid removal surgery
- Advanced-stage endometriosis
- Hysterectomies
- Ovarian cyst removal
- Tubal microsurgical reanastomosis
What is Robot-Assisted Surgery?
Robotic surgery is a bit like a supercomputer system. The surgeon sits at a large computer in the operating room but does not stand over the patient as is the case in conventional surgery. The operating surgeon uses master controls to accurately maneuver surgical instruments connected to the robot’s arms. As a surgeon’s hands and fingers move, the computer translates that movement for the robot to accurately mimic.
The surgeon is in complete control of the process as the robotic system can’t think or move on its own. The surgeon is simply instructing the robot what to do, with the robot having greater precision than a human hand can have by itself. This high level of accuracy is why robotic surgery makes for a great choice for extremely complex and delicate procedures.
Many robotic surgeries are minimal access procedures, also called laparoscopic or keyhole. These procedures are considerably safer and allow for a quicker recovery time for patients than traditional, open surgeries. Minimal access surgeries involve tiny incisions of less than one inch. Large, extensive cuts through the skin, muscle, tissues and nerves are eliminated.
Once the incision(s) are completed, Dr. Jacob directs the robot to insert tiny tubes followed by the necessary surgical instruments and a small, high-definition 3D camera. Throughout the operation, this powerful miniature camera equipment provides Dr. Jacob real-time images on his computer monitor. The images are highly magnified and actually provide a clearer, sharper image than Dr. Jacob would see if he was standing over you in traditional surgery.
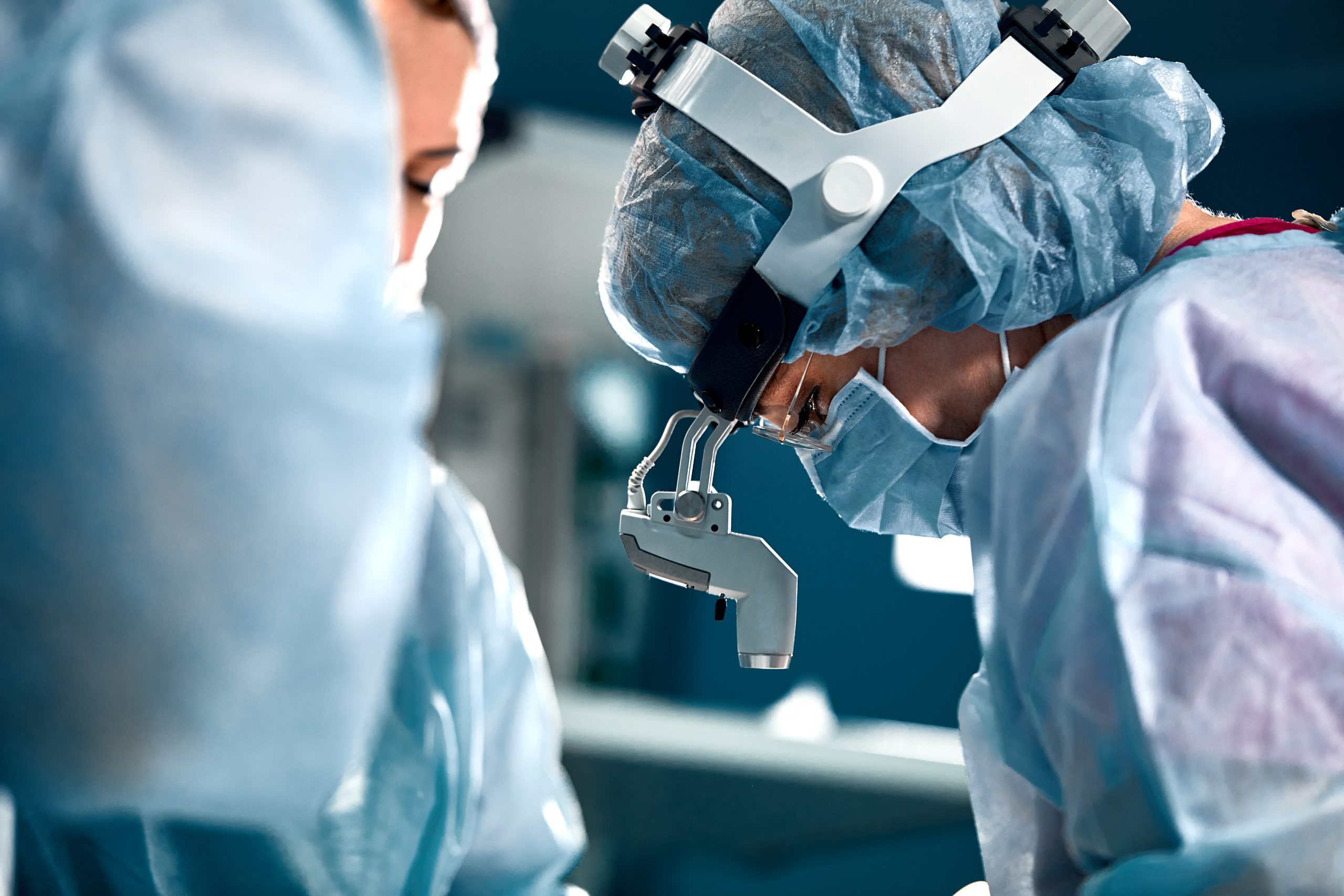

Benefits of Robotic Surgery at GoFertility
In addition to a highly precise procedure completed by a world-class robotic surgeon in Dr. Jacob, robot-assisted surgery has the following advantages compared to conventional, open surgeries:
- Safety: Robotic surgeries result in less loss of blood and reduce the chances of infections
- Less scarring
- Fewer complications
- Post-operation pain reduction: Because Dr. Jacob typically doesn’t cut through muscles or tissues or make large incisions, patients experience less pain in recovery
- Expedited recovery time and shorter hospital stays
- Quicker return to daily life
Additionally, Dr. Jacob has a greater range of motion and dexterity courtesy of the robotic system. He will see a better visual field to allow for a more accurate procedure. He also has improved access to the part of the body being worked on.
Consider Robotic Surgery at GoFertility
While robotics in surgery has existed since the mid-1980s, technological advancements have vastly improved the effectiveness and quality since that timeframe. Currently, the Da Vinci system is the most popular robotic surgical system in American hospitals and is the one Dr. Jacob and GoFertility utilize. Dr. Jacob is heavily involved in robotic surgery research and training other doctors in the field as an industry expert.
Many patients Dr. Jacob has performed robotic surgery on were previously unable to have a baby, especially as it pertains to advanced-stage endometriosis. Endometriosis also causes severe pelvic pain and genital pain that significantly impacts quality of life.
Dr. Jacob and his highly trained team at the Center for Reproductive Medicine and Robotic Surgery are here to help with whatever issues you’re encountering. We’ll guide you through the best next steps to get you feeling healthy again. If robotic surgery is a potential solution for you or can help you in your infertility journey, you can rest assured knowing a world-class surgeon is on your side. Dr. Jacob and our team look forward to the opportunity to serve you. Don’t hesitate to call or email our office with any questions!
