
Advanced Infertility Treatment
As one of the 50 best fertility clinics in the country, GoFertility is a leader in providing an array of solutions for both females and males.
GoFertility (also known as CRMRS) in St. Louis offers industry-leading infertility services for both males and females at our conveniently located office in Creve Coeur. Some of these cutting-edge services include:
- In-vitro fertilization (IVF)
- Ovulation induction
- Intrauterine insemination (IUI)
- Family balancing on embryos
- Intracytoplasmic sperm injection (ICSI)
- Percutaneous epididymal sperm aspiration (PESA)
- Testicular sperm aspiration (TESA)
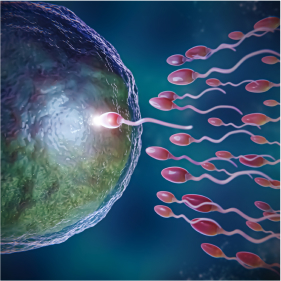
Advanced Infertility Treatments for Females
With 1 in 5 married women 15 to 49 years old with no prior births in the U.S. unable to become pregnant after one year of unprotected sex (CDC), infertility is a nationwide epidemic. You aren’t alone in your infertility journey, and the compassionate team at GoFertility is here to help. We offer IVF, ovulation induction and IUI to our female patients to help them achieve their dream of having a baby.
In-Vitro Fertilization
IVF-ICSI helps infertile females combat such conditions as endometriosis, fibroids or ovulation disorders. During an IVF cycle, mature eggs are collected from the ovaries and injected with a single sperm for fertilization. The eggs are then placed into incubators to allow for fertilization before moving to the cryo tank for freezing. The female’s uterine lining is built up with medication during this cycle before the thawed embryo is transferred into the uterus for ongoing growth.
Ovulation Induction
Hormonal medications are prescribed orally or through injection to encourage the growth and release of eggs in the female patient. These hormonal therapies can improve the number and quality of eggs produced, which increases the likelihood for pregnancy. Our team tracks your progress and response to medication with ultrasounds and blood work to keep you healthy and safe.
Intrauterine Insemination
Sometimes paired with ovulation induction, intrauterine insemination (IUI) occurs when the doctor inserts sperm directly into the female’s uterus to eliminate obstructions. This treatment is particularly beneficial when females have unreceptive cervical mucus or abnormalities in the reproductive organs. It is also helpful when males have a low sperm count or sperm unable to reach the fallopian tubes.
Advanced Infertility Treatments for Males
Male infertility is a factor for about 30 to 40 percent of infertile couples. We view infertility as a “couples problem” and take a comprehensive approach to diagnosing and treating both males and females. Male-specific treatments can include the following.
Intracytoplasmic Sperm Injection (ICSI)
ICSI promotes the best chance for successful egg fertilization, as a male’s single, healthy sperm is selected then injected into a female’s mature egg. More than 70 percent of these eggs then become fertilized at CRMRS, with the resulting embryos placed into the female’s uterus for ongoing growth. ICSI is especially beneficial for severe male infertility cases including low sperm count, low sperm motility and high sperm abnormality.
PESA and TESA
Through PESA (percutaneous epididymal sperm aspiration) or TESA (testicular sperm aspiration), sperm is collected directly from the testis. The procedures are virtually painless, completed quickly, result in immediate recovery and are a fraction of the cost of surgery. In PESA or TESA a fine needle passes through the skin to gather sperm, which is then used fresh or stored frozen in our cryo bank for the future.


What is needed before AI?
Before AI is offered it is important to determine the cause(s) of infertility and a series of tests should be conducted to determine if the couple is a candidate for the procedure. A detailed medical history and physical examination should be conducted initially. The male partner will have two or more semen analysis and a few other tests conducted to estimate the fertilizing ability of his sperm. It is recommended that both be tested for HIV, hepatitis B and C, syphilis, gonorrhea, and chlamydia. In addition, the female partner should be evaluated for rubella and varicella immune status. Also, it is necessary to determine the time and frequency of ovulation using LH surge kits, basal body temperature (BBT) charts and cervical mucus examination.
Some physicians may recommend a Post-coital Test but not much information can be gained from it. Some patients may need a hysterosalpingogram, hysteroscopy or laparoscopy prior to insemination to determine the status of the fallopian tubes, absence of severe adhesions in the pelvic cavity and a reproductive tract free of problems interfering with conception and pregnancy. If your medical history and pelvic exam suggests previous pelvic inflammatory diseases, infections, tubal damage, or endometriosis you will need at least one of those procedures.